Jan 29, Blantyre
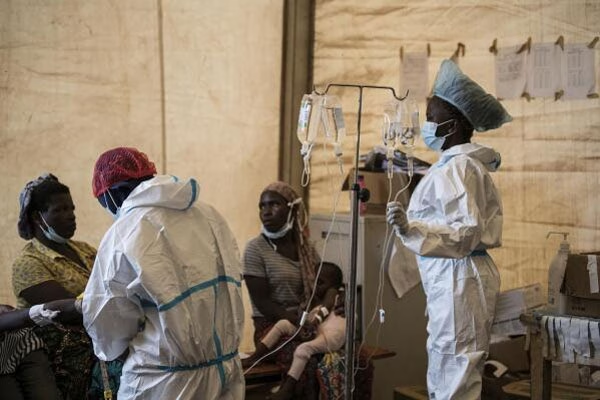
Malawi is facing a renewed public health challenge as cholera cases climb steadily, with the southern commercial city of Blantyre emerging as the epicentre of the outbreak. Since October 2025, health authorities have confirmed more than 50 cholera cases nationwide and at least three related deaths, raising concerns about sanitation gaps, vaccination coverage, and preparedness in densely populated urban areas.
The outbreak gained national attention this week after Malawi’s Minister of Health and Sanitation, Madalitso Baloyi, addressed local leaders during a sensitisation meeting in Blantyre. According to reports by Xinhua News Agency, Blantyre alone has recorded approximately 30 cases and two deaths, accounting for the majority of the country’s current cholera burden. The situation has prompted intensified surveillance, emergency response measures, and appeals for international support.
A Dual Public Health Threat
Compounding the cholera crisis is the recent detection of a case of poliovirus type 2 in Blantyre. Health officials confirmed that samples collected locally were analysed in South Africa, where laboratory testing identified the virus. The case involved a seven-year-old boy who had never been vaccinated, reportedly due to parental beliefs against immunisation.
“This combination of cholera and polio is deeply concerning,” said Gift Kawalazira, Blantyre’s Director of Health and Social Services. “Both diseases thrive where sanitation is poor and vaccination coverage is incomplete. These conditions still exist in many high-density communities.”
While cholera and polio are caused by entirely different pathogens—Vibrio cholerae bacteria and poliovirus, respectively—their co-occurrence highlights overlapping vulnerabilities in water, sanitation, hygiene (WASH), and routine immunisation systems.
Understanding Cholera and Why It Spreads
Cholera is an acute diarrhoeal illness transmitted through contaminated water or food. According to the World Health Organization (WHO), it can cause severe dehydration and death within hours if left untreated, though it is easily preventable and treatable with prompt care. Globally, WHO estimates 1.3 to 4 million cholera cases and up to 143,000 deaths each year, largely in low-resource settings.
In Malawi, recurrent cholera outbreaks have historically been linked to unsafe drinking water, inadequate sanitation infrastructure, flooding, and population displacement. Blantyre’s rapid urbanisation has created crowded informal settlements where access to clean water and toilets remains limited, increasing the risk of faecal contamination of water supplies.
“Cholera is not just a medical issue—it is a social and infrastructural one,” said Dr. Thokozani Mbewe, a public health specialist at the University of Malawi College of Medicine, who is not involved in the current response. “When sanitation systems fail, bacteria spread quickly, especially during rainy seasons.”
Government and International Response
In response to the rising cases, the Malawian government has activated its National Public Health Emergency Operations Centre and established a national incident management team to coordinate surveillance, case management, and risk communication. Authorities are also working closely with international partners, including WHO and the United Nations Children’s Fund (UNICEF), to scale up vaccination campaigns, water chlorination, and community awareness efforts.
Last December, Malawi appealed for more than $3 million to support its Cholera Preparedness and Control Plan. The total budget for the plan stands at $3.37 million, but officials report that only about $357,000 has been secured so far, leaving a funding gap exceeding $3 million.
“This shortfall directly affects our ability to respond quickly and comprehensively,” Minister Baloyi said at a press briefing in Lilongwe. “Resources are needed for treatment supplies, oral cholera vaccines, clean water interventions, and public education.”
Cross-Border Risks and Regional Coordination
Health officials have also intensified cross-border collaboration with neighbouring Mozambique, particularly in the border districts of Mwanza in Malawi and Moatize in Mozambique. Joint investigations are underway to track suspected cases and reduce cross-border transmission, a known risk factor in previous regional outbreaks.
“Pathogens do not respect national borders,” noted Dr. Patrick Kumwenda, an infectious disease epidemiologist based in Lilongwe. “Regional coordination is essential, especially in areas with frequent population movement.”
Implications for Public Health and Communities
For the general public, the outbreak underscores the importance of basic preventive measures. Health authorities are urging residents to boil or chlorinate drinking water, wash hands regularly with soap, use latrines, and seek medical care immediately if symptoms such as watery diarrhoea and vomiting occur.
Vaccination also remains a cornerstone of prevention. Oral cholera vaccines can significantly reduce the risk of severe disease during outbreaks, while routine childhood immunisation protects against polio and other preventable illnesses.
“Vaccines are among the most effective public health tools we have,” said Dr. Mbewe. “The polio case in Blantyre is a reminder that gaps in immunisation—often driven by misinformation or access issues—can reverse years of progress.”
Limitations and Ongoing Challenges
Despite intensified efforts, challenges remain. Surveillance data may underestimate the true number of cases, as mild infections often go unreported. Funding constraints limit the scale of interventions, and behavioural change around hygiene practices can take time.
Some experts caution against panic, noting that cholera outbreaks, while serious, are controllable with proven strategies. “With early detection, rehydration therapy, and community engagement, mortality can be kept very low—often below one percent,” Dr. Kumwenda said.
Looking Ahead
As Malawi works to contain the outbreak, sustained investment in water and sanitation infrastructure, health education, and vaccination programmes will be critical to preventing future surges. Public cooperation, health officials stress, will play a decisive role.
“This is a moment for collective responsibility,” Minister Baloyi said. “If communities, government, and partners work together, we can stop the spread and protect our most vulnerable citizens.”
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
https://www.daijiworld.com/index.php/news/newsDisplay?newsID=1305027