In a powerful call to action timed with the first-ever World Cervical Cancer Elimination Day, the World Health Organization (WHO) has urged Southeast Asian countries to ramp up their efforts against cervical cancer—a disease that claims one woman’s life every two minutes globally. Despite being both preventable and treatable, cervical cancer continues to exert a heavy toll on women across this region, which shoulders nearly one-fourth of the world’s cases.
Lead: A Crisis Unfolding in Southeast Asia
According to WHO data, 160,000 new cervical cancer cases and 100,000 related deaths were recorded in Southeast Asia alone in 2022. This means that every two minutes, somewhere in the world, another woman loses her life to a disease that can often be stopped before it starts. These numbers have prompted international health authorities to call for urgent steps to bridge gaps in vaccination, screening, and treatment.
Key Findings & Recent Developments
Health leaders cite glaring disparities in prevention and care. Bhutan is a regional example, already meeting all 2030 WHO goals for elimination: 90% HPV vaccination among girls by age 15, screening 70% of women at ages 35 and 45, and ensuring access to treatment for 90% of those diagnosed. Thailand’s Cancer Anywhere initiative is another bright spot, increasing treatment availability. Nevertheless, eight other regional countries offer nationwide HPV vaccination programs and six feature population-based screening, but coverage and follow-through remain far below what is needed.
Dr. Catharina Boehme, Officer-in-Charge, WHO South-East Asia, emphasized the urgency: “The disease continues to claim a woman’s life every two minutes globally. We must accelerate efforts to meet the WHO’s 2030 elimination targets and ensure that no woman dies from cervical cancer or other preventable diseases.”
Context: The Preventable Nature of Cervical Cancer
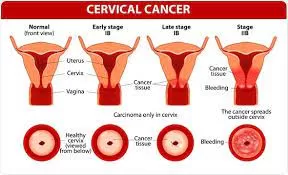
Cervical cancer is primarily caused by persistent infection with high-risk strains of the human papillomavirus (HPV), with the vast majority of cases arising from this source according to the Centers for Disease Control and Prevention and the International Agency for Research on Cancer. The disease is most often detected through screening methods such as Pap tests and HPV DNA testing, which can find pre-cancerous changes before they progress.
Vaccination is a proven prevention tool. The HPV vaccine, recommended for girls and young women ideally before the onset of sexual activity, provides strong protection against the most dangerous HPV types. Treatments for cervical precancer and invasive cancer also exist, including excisional procedures, radiotherapy, and chemotherapy, but their availability varies sharply by country and by socioeconomic status.
Expert Commentary
Dr. Neha Shrivastava, a gynecologic oncologist at All India Institute of Medical Sciences (not involved in WHO’s work), comments: “Routine screening and vaccination are game-changers. We see dramatic reductions in cervical cancer rates where these interventions are widely adopted. However, health systems must also ensure that women diagnosed with abnormal results receive timely and effective treatment.”
Implications for Public Health
The WHO’s recommended strategy is three-pronged:
-
Vaccinate 90% of girls against HPV by age 15
-
Screen 70% of women at ages 35 and 45 using high-performance methods
-
Treat 90% of women identified with pre-cancer and cancer
If implemented, these steps could shift the trajectory of cervical cancer in Southeast Asia and globally. Governments are encouraged to capitalize on affordable single-dose vaccine regimens, expand screening (including self-sampling options), and integrate these services into general reproductive health frameworks. Universal health coverage is pivotal to reaching women who may otherwise be missed.
Bhutan’s achievement of WHO targets shows what is possible with concerted political will and investment. In contrast, fragmented efforts or under-resourced programs risk stalling progress and perpetuating preventable deaths.
Limitations and Counterarguments
Despite this momentum, barriers remain. HPV vaccine hesitancy (often due to misinformation), uneven screening uptake, and limited access to multidisciplinary treatment centers weaken comprehensive responses. Funding constraints, logistical challenges, and cultural attitudes further impact rollout effectiveness.
Some critics also caution against relying solely on vaccination, emphasizing equally robust investments in education, screening, and post-diagnosis care to ensure women are not left behind at any step.
Practical Implications for Readers
For individuals, the core message is clear:
-
If eligible for HPV vaccination, getting immunized early provides substantial protection.
-
Routine cervical cancer screening can detect changes before they become life-threatening.
-
Seek medical advice and regular checkups; recognize the value of cancer prevention as part of overall wellbeing.
Public health agencies and professionals must continue education campaigns that address vaccine hesitancy and misconceptions, making screening and care accessible to all communities.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
World Health Organization (2022), “Cervical cancer kills one woman every two minutes, WHO urges South-East Asia to act,” Economic Times Health, Nov 2025.