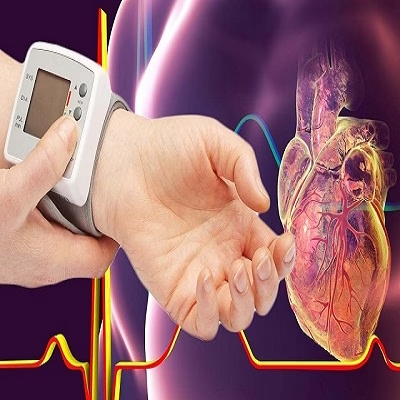
Central blood pressure (CBP) is emerging as a more precise clinical marker than traditional brachial blood pressure (bBP) for assessing cardiovascular risk, particularly in relation to aortic and vascular diseases. Recent studies show that CBP more accurately reflects the pressure on central arteries, correlates better with arterial stiffness, thoracic aortic aneurysm (TAA) growth, and cardiovascular events, offering deeper insights into cardiac workload and risk stratification than peripheral brachial measurements.
Central vs. Brachial Blood Pressure: Defining the Difference
Brachial blood pressure, the common measurement taken at the arm, represents peripheral arterial pressure. In contrast, central blood pressure measures the pressure in the aorta and other major arteries near the heart, directly reflecting the load on central arteries exposed to cardiac output. This difference is critical because the pressure experienced by organs and the aortic wall is more accurately captured by central measures than by peripheral readings, which are influenced by wave reflections and arterial properties downstream.
Key Findings on Cardiovascular Risk Prediction
Multiple studies have demonstrated that central blood pressure parameters, including central systolic blood pressure (cSBP) and central pulse pressure (cPP), better predict cardiovascular outcomes compared to brachial blood pressure. For example, a large cohort analysis found that patients with isolated central hypertension had significantly elevated risks of cardiovascular and cerebrovascular events compared to those with isolated brachial hypertension or concordant hypertension status. Central hypertension showed a hazard ratio of approximately 2.28 for primary cardiovascular endpoints versus normotension, suggesting a stronger association with adverse events independent of brachial pressure readings.
Meta-analyses corroborate these findings, showing that for every 10 mm Hg increase in cSBP, the risk for composite cardiovascular endpoints rises by about 14%, with similar increments for cardiovascular mortality. This predictive value remains after adjusting for brachial blood pressure, reinforcing the independent and additive utility of central pressure measurements in risk assessment.
Central Blood Pressure and Thoracic Aortic Aneurysm (TAA)
TAA is a life-threatening dilation of the thoracic aorta, with hypertension being a major risk factor for aneurysm growth and rupture. Recent evidence highlights that central blood pressure, not brachial pressure, correlates better with aneurysm size and progression. Patients without clinical hypertension diagnosis (based on brachial measures) but elevated cSBP and cPP show larger aneurysms and faster aneurysm expansion during follow-up, underscoring the sensitivity of central pressure in detecting vascular stress leading to aneurysm development. The aortic wall stress, heightened by central systolic load, fuels TAA growth, a process inadequately captured by brachial pressure alone.
Expert Perspectives
Dr. Michael Roman, a cardiology expert in vascular biomechanics, states, “Central blood pressure reflects the true mechanical load on the aorta and heart better than brachial readings, making it a crucial parameter for refining cardiovascular risk prediction and management.” Independent experts emphasize that incorporating central hemodynamic indices into clinical protocols could lead to more tailored and effective hypertension therapies, potentially reducing morbidity from aortic and cardiovascular diseases.
Implications for Public Health and Clinical Practice
Incorporating central blood pressure measurement into routine clinical practice promises to enhance risk stratification for cardiovascular and aortovascular diseases, allowing earlier intervention and more precise treatment adjustments. Novel non-invasive technologies using pulse wave analysis to estimate CBP are becoming more accessible, facilitating broader adoption beyond research settings.
Public health strategies focused on blood pressure control may benefit from considering central pressure targets, particularly in patients with known aortic conditions or high cardiovascular risk. This approach aligns with findings from landmark trials showing that intensive blood pressure lowering reduces cardiovascular events, highlighting the importance of accurate pressure measurement.
Limitations and Counterarguments
Despite evidence supporting CBP’s superiority, some studies report that central and brachial blood pressures provide comparable risk prediction in certain populations. Measurement standardization remains an issue, with different devices and calibration methods potentially influencing CBP values, leading to variability. Further, large-scale prospective trials are needed to confirm whether targeting central pressure in treatment protocols yields better outcomes compared to brachial pressure-based strategies.
Conclusion
Central blood pressure represents a promising biomarker that enhances understanding of cardiovascular risk beyond what brachial blood pressure offers, particularly for vascular conditions such as thoracic aortic aneurysm. Its greater association with arterial stiffness and cardiovascular events highlights the need for clinicians to reevaluate current hypertension assessment models. Ongoing research and technological advances will be crucial to fully integrate central blood pressure monitoring into everyday clinical care, potentially transforming the management of hypertensive and aortovascular diseases.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: