March 3, 2026
ATLANTA — In a critical move to address the most significant public health challenge of the year, Jay Bhattacharya, MD, PhD, acting director of the U.S. Centers for Disease Control and Prevention (CDC), issued an urgent appeal on March 2, 2026, for Americans to prioritize the measles-mumps-rubella (MMR) vaccine. Speaking via a video address on X (formerly Twitter), Dr. Bhattacharya characterized the vaccine as the “most reliable and effective” tool to combat an escalating measles crisis that has seen 1,136 confirmed cases across 28 jurisdictions as of late February. With outbreaks spreading rapidly in states like Arizona, California, Florida, and South Carolina, the CDC is now deploying emergency technical staff, laboratory support, and medical therapeutics to the hardest-hit regions to prevent the U.S. from losing its hard-won “measles-eliminated” status.
A Nation at a Crossroads: The 2026 Outbreak
The United States is currently grappling with a measles resurgence of a scale not seen in decades. The 1,136 cases confirmed in the first eight weeks of 2026 represent nearly half of the total cases recorded in all of 2025 (approximately 2,300).
The epicenter of the current crisis is South Carolina, which has reported over 600 cases since October 2025. The situation there has led to 18 hospitalizations and forced the quarantine of students and staff at more than 20 schools. This level of community transmission is particularly alarming to health officials because it suggests the virus is circulating freely among the unvaccinated population rather than being limited to isolated travel-related incidents.
According to CDC data, 90% of this year’s cases are linked to ten distinct outbreaks, and 92% of those infected were either unvaccinated or under-vaccinated. Public health experts warn that if this local transmission persists for more than 12 consecutive months, the Pan American Health Organization (PAHO) may revoke the U.S. status as a country that has eliminated measles—a benchmark the nation has maintained since 2000.
The Pivot Toward Prevention
Dr. Bhattacharya’s endorsement of the MMR vaccine marks a significant moment in federal health communication. Having assumed the acting directorship in February 2026 while simultaneously leading the National Institutes of Health (NIH), Bhattacharya’s stance offers a clear directive following a period of shifting federal guidance.
“There is no cure for measles, which is why prevention is so critical,” Bhattacharya stated in his address. “The MMR vaccine remains the most reliable and effective way to prevent it. Two doses offer 97% efficacy in lifelong protection against measles and complications.”
This messaging stands in contrast to the skepticism previously voiced by some figures in the current administration, including Health Secretary Robert F. Kennedy Jr., who has historically questioned the broader necessity of certain childhood immunizations. While Bhattacharya has been a vocal critic of mandates for newer vaccines like those for COVID-19, his current defense of the MMR vaccine emphasizes its decades-long track record of safety and its role in maintaining “herd immunity.”
Understanding the Virus and the Vaccine
Measles is a highly contagious paramyxovirus. It is so infectious that if one person has it, up to 90% of the people close to them who are not immune will also become infected.
The Clinical Reality of Measles
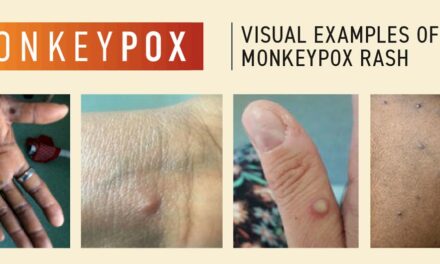
Measles is often dismissed as a simple childhood rash, but medical experts emphasize its severity:
-
Initial Symptoms: High fever, cough, coryza (runny nose), and conjunctivitis.
-
Complications: Approximately 1 in 20 children with measles develops pneumonia; 1 in 1,000 develops encephalitis (brain swelling), which can lead to permanent neurological damage.
-
The “Immune Amnesia”: Research suggests that measles can “reset” the immune system, making children more vulnerable to other bacterial and viral infections for years after recovery.
The Efficacy of MMR
The MMR vaccine is a live-attenuated vaccine administered in two doses.
-
Dose 1: Typically given at 12–15 months of age; provides ~93% protection.
-
Dose 2: Given at 4–6 years of age; increases protection to 97%.
A 2017 study published in BMJ Paediatrics Open highlighted that while unvaccinated children faced a 0.4% hospitalization rate during outbreaks, that rate dropped to zero among those who had received both doses.
Expert Perspectives: A Welcome Realignment
The public health community has largely reacted with relief to the CDC’s firm stance.
“This is a welcome pivot toward evidence-based messaging when outbreaks demand it,” said Dr. Katelyn Winter, an independent epidemiologist. “When you see cases accelerating this quickly, there is no room for ambiguity.”
Dr. Sean O’Leary, a pediatric infectious disease specialist at the University of Colorado, echoed this sentiment: “Two doses of MMR are 97% effective, and reaffirming this saves lives—especially with 1,136 cases already threatening our elimination status.”
However, the conversation remains complex. Groups such as Physicians for Informed Consent have raised concerns, arguing that natural infection can provide more robust, long-term immunity and pointing to potential side effects such as fever or rare allergic reactions.
Dr. Bhattacharya acknowledged these viewpoints by framing vaccination as a personal but recommended choice. “I recognize health choices are personal; discuss with your doctor,” he noted, attempting to bridge the gap between public health necessity and the administration’s emphasis on individual medical autonomy.
Practical Implications for Families
As the CDC ramps up resources, what does this mean for the average household? Public health officials recommend three immediate steps:
-
Verify Records: Check immunization records for yourself and your children. If you cannot find them, a simple blood test (titer) can confirm immunity.
-
Catch-Up Vaccines: If a dose was missed, it is safe and effective to receive the MMR vaccine at any age.
-
Monitor Travel Advisories: With measles surging globally, ensure your family is protected before traveling internationally or to domestic “hot spots” like South Carolina or Arizona.
Addressing Limitations and Risks
While the MMR vaccine is among the most studied medical interventions in history, it—like all medicines—is not without risks.
-
Side Effects: Mild fever or a temporary rash occur in about 5–15% of recipients.
-
Serious Adverse Events: Severe allergic reactions occur in approximately 1 in 1,000,000 doses.
-
Waning Immunity: Some studies suggest a very slight wane in protection over decades (roughly 0.04% annually), but the two-dose series remains the gold standard for lifelong protection.
The CDC maintains that the risks of the disease—which can be fatal—vastly outweigh the risks of the vaccine. While no deaths have been reported in the U.S. so far in 2026, the rising hospitalization rate is a lagging indicator that has doctors on high alert.
Looking Ahead
The primary challenge remains reaching “pockets” of under-vaccinated communities where coverage has fallen below the 95% threshold required for herd immunity. As Dr. Bhattacharya navigates his dual role at the CDC and NIH, the stability of these vaccination policies will be closely watched by both healthcare providers and a wary public.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Reuters. “CDC acting director Bhattacharya backs use of measles vaccine.” March 2, 2026.