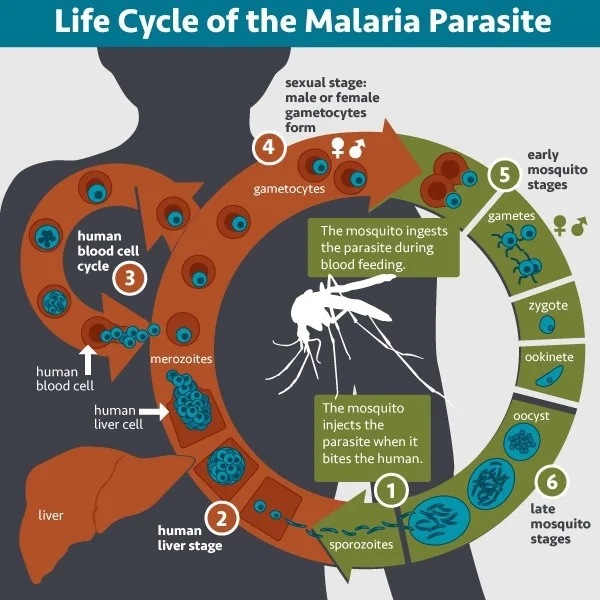
The antiparasitic drug ivermectin, long used to combat river blindness and lymphatic filariasis, is now drawing global attention as research uncovers its surprising potential to curb malaria transmission. In July 2025, major studies published in The New England Journal of Medicine and supported by leading research organizations revealed that monthly ivermectin administration led to a significant 26% reduction in malaria incidence among children in Kenya—an area already benefiting from widespread use of insecticide-treated bed nets. This development marks a milestone in the fight against a disease that caused 263 million cases and nearly 600,000 deaths globally in 2023, particularly as insecticide resistance and mosquito behavioral changes threaten progress.
Key Findings From Recent Studies
The BOHEMIA trial, the largest investigation of ivermectin for malaria to date, involved nearly 29,000 residents in Kwale County, Kenya. Children aged 5 to 15 received a monthly dose of ivermectin (400 micrograms/kg) for three months. The control group received albendazole, a common anti-worming agent. Researchers confirmed both drugs were safe, but ivermectin yielded a 26% reduction in malaria cases compared to controls—a result surpassing the World Health Organization’s efficacy benchmark for new vector-control tools.
By killing mosquitoes that feed on treated individuals, ivermectin works through a novel mechanism distinct from standard insecticides. Modeling analyses suggest that mass drug administration (MDA) campaigns covering 12.5%-50% of a population could avert as many as 288 malaria cases per 1,000 people and save significant disability-adjusted life years, especially in high-transmission settings in sub-Saharan Africa.
Expert Perspectives
Carlos Chaccour, MD, PhD, co-principal investigator of the BOHEMIA project, commented, “Ivermectin has shown great promise in reducing malaria transmission and could complement existing control measures. With continued research, ivermectin MDA could become an effective tool for malaria control and even contribute to elimination efforts.”
Dr. Joseph Mwangangi, Senior Principal Research Scientist at KEMRI-Wellcome Trust, highlighted, “These results align with WHO criteria for new vector control tools and suggest a real opportunity to strengthen malaria prevention where traditional methods are failing.”
An independent view comes from Professor Richard Steketee, MD, MPH, who noted in a NEJM editorial that “seasonal mass administration of ivermectin on a monthly schedule can align with other malaria or health interventions, providing substantial reductions in transmission. Dosing schedules and program delivery will be key challenges going forward.”
Context and Background
Malaria control has historically relied heavily on insecticide-treated bed nets and indoor spraying. While highly effective, these strategies are now encountering rising resistance among mosquito populations, as well as adaptive changes that diminish their impact. Ivermectin’s unusual property—it makes human blood toxic to mosquitoes for days after ingestion—has enabled scientists to explore mass drug administration as a complementary intervention. Previous trials in Burkina Faso and modeling studies indicate its capability to kill both mosquitoes and parasites, amplifying the potential utility for regions struggling with malaria control.
Implications for Public Health
If integrated into national malaria control programs, ivermectin could offer several practical benefits:
-
Supplement existing tools: Especially where insecticide resistance threatens bed net efficacy.
-
Mass campaigns: MDA has demonstrated safety, even at relatively large scales in Kenya and modeled scenarios in sub-Saharan Africa.
-
Outdoors coverage: Targets transmission beyond the home, as mosquitoes increasingly feed outdoors.
However, deployment would require careful scheduling, sustained funding, and vigilance for potential side effects or resistance. The intervention could be particularly transformative in places where malaria remains endemic year-round and current protocols are losing ground.
Potential Limitations and Counterarguments
Experts raise several caveats:
-
Magnitude of impact: The 26% reduction is meaningful but may not be sufficient on its own in areas with intense transmission.
-
Safety profile: While recent research points to safety at the tested doses, long-term effects and the risk of resistance must be monitored.
-
Program challenges: Monthly administration demands robust public health infrastructure. More frequent dosing or the development of longer-acting drugs could further boost efficacy, but these strategies need additional evaluation.
-
Environmental effects: Some ecotoxicological analyses caution about potential risks to non-target species and broader environmental impacts when ivermectin is used widely.
-
Conflicting evidence: Some studies, such as trials adding ivermectin to other antimalarial regimens, found no added benefits in certain settings, highlighting the need for tailored approaches.
Practical Implications for Readers
For health professionals:
-
Stay informed about evolving research and policy recommendations regarding ivermectin and its role in malaria prevention.
-
Educate patients in high-risk areas about upcoming interventions and the importance of sustained vector control.
-
Monitor for updates from WHO and national health authorities on program rollout.
For health-conscious consumers:
-
Understand that ivermectin is not a replacement for standard malaria prevention (bed nets, indoor spraying) but could be an additional layer of protection in select regions.
-
Follow local health advisories; do not self-administer ivermectin for malaria prevention outside approved campaigns.
-
Advocate for responsible and evidence-based use of new interventions to maximize community benefits and minimize risks.
Conclusion
Ivermectin’s potential to interrupt malaria transmission is supported by robust, peer-reviewed research demonstrating a substantial reduction in new infections among children when administered monthly. While its integration into malaria control strategies offers hope amid challenges like insecticide resistance, further trials, long-term studies, and careful monitoring will be necessary to optimize impact and safety. Authorities recommend considering ivermectin MDA as a supplemental—not replacement—tool alongside existing measures, under rigorous public health oversight.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://www.ndm.ox.ac.uk/news/new-research-supports-ivermectin-as-an-effective-strategy-to-control-malaria-transmission
- https://malariaworld.org/news/new-research-supports-ivermectin-as-an-effective-strategy-to-control-malaria-transmission