February 7, 2026
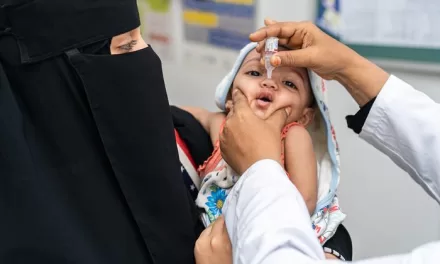
NEW DELHI — In a sweeping effort to dismantle the geographic and socioeconomic barriers that have historically sidelined India’s most vulnerable populations, the Ministry of Health and Family Welfare has announced a comprehensive expansion of healthcare infrastructure targeting tribal and remote regions. Under the National Health Mission (NHM), the government is deploying a multi-pronged strategy—combining relaxed infrastructure norms, a massive surge in digital teleconsultation, and mobile medical fleets—to ensure that quality healthcare is no longer a privilege of the urban elite, but a guaranteed right for the “last mile” citizen.
A New Era of Accessibility
For decades, the rugged terrain of India’s hilly and tribal belts posed a logistical nightmare for healthcare delivery. Standard population-based norms often left small, isolated hamlets without a local clinic. Today, the Ministry confirmed a pivotal shift: norms for establishing health centers have been significantly relaxed.
In tribal and “hard-to-reach” areas, the population threshold for a Sub Health Centre (SHC) has been lowered to 3,000 (down from 5,000), and for Primary Health Centres (PHCs) to 20,000 (down from 30,000). This regulatory adjustment has paved the way for 1.82 lakh Ayushman Arogya Mandirs (AAMs) to become operational nationwide, with over 30,800 specifically situated in 178 tribal districts.
“This isn’t just about building walls; it’s about changing the definition of proximity,” says Dr. Ananya Sharma, a public health policy expert (unaffiliated with the Ministry). “By lowering the population barrier, the government is acknowledging that a person’s right to health should not be dictated by the difficulty of the terrain they inhabit.”
Tech and Triage: The Digital Lifeline
Perhaps the most transformative element of this expansion is the integration of the Ayushman Bharat Digital Mission (ABDM). As of late 2025, the government reported a staggering 42.66 crore teleconsultations conducted through AAMs.
This digital infrastructure allows a patient in a remote village in Odisha or Ladakh to consult with a specialist in a metropolitan hospital via video link. This “hub-and-spoke” model addresses the chronic shortage of specialist doctors in rural areas, providing a continuum of care that was previously non-existent.
Key Infrastructure Milestones:
| Facility Type | Nationwide Total | Tribal District Specifics |
| Ayushman Arogya Mandirs | 1.82 Lakh | 30,817 |
| Critical Care Blocks (PM-ABHIM) | – | 110 Approved |
| Integrated Public Health Labs | – | 168 Approved |
| Mobile Medical Units (MMUs) | 1,477 | 763 (PM-JANMAN specific) |
Specialized Care for Vulnerable Groups
The PM-JANMAN (Pradhan Mantri Janjati Adivasi Nyaya Maha Abhiyan) initiative, launched in late 2023, has further intensified focus on Particularly Vulnerable Tribal Groups (PVTGs). The mission has authorized up to 10 Mobile Medical Units (MMUs) per district in these areas, compared to just two in plain districts. These “hospitals on wheels” provide essential screenings, vaccinations, and basic curative services directly to the doorstep of those who cannot travel.
Furthermore, the RMNCAH+N strategy (Reproductive, Maternal, Newborn, Child, Adolescent Health Plus Nutrition) is making significant inroads in maternal health. By utilizing Accredited Social Health Activists (ASHAs)—with one ASHA now permitted per habitation regardless of population size—the mission has seen a rise in institutional deliveries through the Janani Suraksha Yojana (JSY).
Expert Perspectives and Challenges
While the scale of the rollout is unprecedented, independent experts urge a focus on long-term sustainability. “The infrastructure is a massive leap forward,” notes Dr. Rajesh Varma, a former consultant for international health organizations. “However, the next challenge is ‘human infrastructure.’ Ensuring that these remote centers remain staffed with trained professionals who are culturally sensitive to tribal communities is the key to actualizing these gains.”
Critics also point out that while teleconsultation is a powerful tool, it relies heavily on stable internet connectivity, which remains intermittent in deep forest or high-altitude zones. The Ministry’s response has been the strengthening of physical infrastructure through the Pradhan Mantri Ayushman Bharat Health Infrastructure Mission (PM-ABHIM), which has a budget of ₹64,180 crore to build critical care hospital blocks and labs that can operate independently of digital links.
What This Means for the Public
For the average citizen in a remote region, these developments mean:
-
Reduced Travel Costs: Fewer “out-of-pocket” expenses for traveling to distant cities for basic specialist advice.
-
Faster Emergency Response: The 110 approved Critical Care Blocks are designed to handle life-threatening situations closer to home.
-
Comprehensive Records: Through ABDM, patients will have a longitudinal electronic health record, ensuring that their medical history follows them, regardless of where they seek treatment.
As the government continues its annual Common Review Missions (CRM) to monitor these programs, the focus remains on “Health for All.” The transition from traditional clinics to Ayushman Arogya Mandirs represents a shift toward a more holistic, preventive, and accessible healthcare ecosystem.
References
-
Official Source: Ministry of Health and Family Welfare, Government of India. Press Information Bureau (PIB) Delhi, Feb 6, 2026.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.