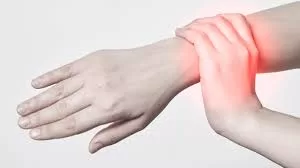
For decades, the medical community viewed the debilitating nerve pain caused by chemotherapy as an unfortunate, direct side effect of toxic drugs “poisoning” the nervous system. However, a groundbreaking study published in Science Translational Medicine reveals a different culprit: the patient’s own immune system.
The research, led by teams at Weill Cornell Medicine and Wake Forest University School of Medicine, identifies a specific molecular stress response within immune cells that triggers a cascade of inflammation and subsequent nerve injury. This discovery not only explains why up to 50% of chemotherapy patients suffer from tingling, numbness, and searing pain—known as chemotherapy-induced peripheral neuropathy (CIPN)—but also offers a roadmap for preventing it with drugs already entering clinical trials.
The “Alarm System” That Backfires
At the heart of the discovery is a biological pathway called IRE1α-XBP1. Under normal conditions, this pathway acts as an internal monitor, helping cells manage stress. However, when cancer patients receive taxane-based chemotherapies like paclitaxel, the drug causes immune cells to produce “reactive oxygen species”—essentially highly reactive molecules that put the cell under intense oxidative stress.
This stress flips the IRE1α switch into overdrive. Instead of helping the cell recover, the overactive pathway transforms common white blood cells into “inflammatory messengers.”
“We uncovered a molecular mechanism that maps specifically to immune cells, not neurons,” explains co-senior author Dr. Juan Cubillos-Ruiz, the William J. Ledger, M.D. Distinguished Associate Professor at Weill Cornell Medicine. “This provides strong evidence that chemotherapy-induced neuropathy is not just a nerve issue but an immune-mediated inflammatory process.”
From Immune Cells to Nerve Damage
The study utilized mouse models that accurately replicate the human experience of CIPN. Researchers tracked the journey of these stressed immune cells as they migrated toward the dorsal root ganglia—clusters of sensory nerve cells located near the spinal cord that act as the gateway for pain signals from the limbs.
Once they arrive, these “angry” immune cells release a flood of inflammatory signals. These signals bombard the nearby nerves, leading to:
-
Degeneration of nerve fibers.
-
Hypersensitivity to cold (a hallmark of CIPN).
-
Persistent burning or tingling sensations in the hands and feet.
By identifying this “biological chain reaction,” researchers have shifted the focus of treatment from the nerves themselves to the immune cells that are attacking them.
A Two-Fold Victory: Fighting Cancer and Pain
The most promising aspect of the research lies in the potential for prevention. When the team used a drug to block the IRE1α signal in mice, the results were striking: the surge of inflammation vanished, and the mice were protected from nerve damage while still receiving the life-saving chemotherapy.
Crucially, IRE1α inhibitors are already being studied in Phase 1 clinical trials for treating advanced solid tumors. Because cancer cells often hijack this same stress pathway to grow and resist treatment, a single drug could theoretically perform a “double duty”: making the chemotherapy more effective at killing the tumor while shielding the patient’s nerves from side effects.
“Targeting IRE1α… could mitigate neuropathy induced by taxanes, helping patients continue with their chemotherapy without the negative side effects,” says Dr. Cubillos-Ruiz.
Predicting the Vulnerable
For many patients, the fear of permanent nerve damage leads to difficult decisions, such as reducing chemotherapy doses or stopping treatment entirely. This new research may soon provide a way to predict who is most at risk before the first dose is even administered.
In a pilot study of women with gynecologic cancers, researchers analyzed blood samples taken before and during chemotherapy. They found that patients who eventually developed severe CIPN had higher activity in the IRE1α-XBP1 pathway in their blood even before physical symptoms appeared. This suggests that a simple blood test could one day allow oncologists to identify high-risk patients and provide preventive “nerve-shielding” therapies.
Expert Perspective and Limitations
While the results are being hailed as a significant step forward, independent experts urge cautious optimism.
“The transition from mouse models to human clinical standards is a steep climb,” says Dr. Elena Rossi, a clinical neurologist not involved in the study. “While the pilot data in humans is encouraging, we need larger, multi-center trials to confirm that blocking this pathway doesn’t interfere with the overall immune response needed to fight secondary infections during chemotherapy.”
Additionally, the study focused primarily on taxanes (like paclitaxel). It remains to be seen if other classes of chemotherapy drugs, such as platinum-based agents (cisplatin) or vinca alkaloids, trigger the same IRE1α-XBP1 stress response.
What This Means for Patients
For the millions of cancer survivors living with chronic “pins and needles” or debilitating pain, this research validates that their symptoms are rooted in a specific biological process rather than being an unavoidable consequence of treatment.
If the clinical trials for IRE1α inhibitors prove successful, the future of cancer care could involve a “supportive oncology” approach:
-
Screening: A pre-treatment blood test to assess immune stress levels.
-
Protection: Administering a pathway inhibitor alongside chemotherapy.
-
Completion: Allowing patients to finish their full course of treatment without dose reductions due to pain.
As research moves into human trials, the hope is that the next generation of cancer survivors will not have to trade their long-term neurological health for their lives.
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References and Sources
New Discovery May Prevent Debilitating Chemotherapy Nerve Pain