NEW YORK — As millions worldwide continue to grapple with the lingering effects of the SARS-CoV-2 virus, a groundbreaking study from the NYU Grossman School of Medicine has identified a startling structural link between Long COVID and Alzheimer’s disease. Researchers found that individuals suffering from persistent post-COVID symptoms exhibit significant enlargement of the choroid plexus, a vital brain structure responsible for waste clearance and immune surveillance.
The study, published in early February 2026 in the journal Alzheimer’s & Dementia, suggests that the “brain fog” reported by Long COVID patients may be more than a temporary cognitive cloud. Instead, it may share the same underlying biological “clogging” mechanisms that characterize the early stages of dementia.
The Brain’s Clogged Pipes: Key Findings
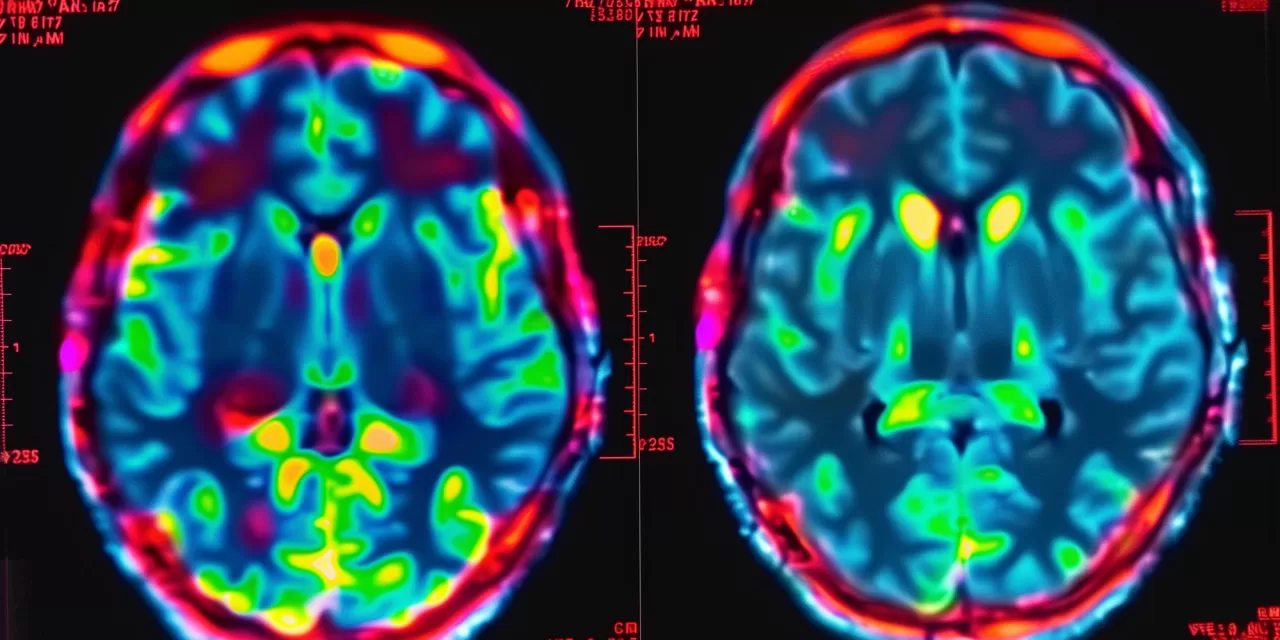
The research team, led by NYU radiologists and neurologists, analyzed brain MRI scans from 179 participants, including those with Long COVID, those who recovered fully, and healthy controls.
The data revealed that Long COVID patients had a 10% larger choroid plexus (ChP) volume compared to their healthy counterparts. Perhaps more concerning was the discovery that this enlargement was coupled with a reduction in cerebral blood flow—a hallmark of vascular remodeling driven by chronic inflammation.
To understand the significance, experts suggest using a “plumbing” analogy. The choroid plexus acts as the brain’s filtration and fluid production system, creating cerebrospinal fluid (CSF) that washes away toxic metabolic waste, such as amyloid-beta plaques.
“Think of the ChP as the brain’s plumbing system,” says the study’s authors. When this system becomes inflamed or scarred—a process known as stromal fibrosis—it acts like a rusty pipe buildup. Toxins that should be flushed out of the brain instead become trapped, fueling a cycle of neuroinflammation and cognitive decline.
The Biomarker Connection
The study didn’t just look at structure; it looked at blood chemistry. Researchers found that ChP volume positively correlated with two specific blood biomarkers:
-
pTau217 (Phosphorylated Tau): A protein heavily associated with the progression of Alzheimer’s disease.
-
GFAP (Glial Fibrillary Acidic Protein): A marker of brain injury and astrocyte activation (inflammation).
Clinical assessments mirrored these biological findings. Patients with the largest choroid plexus measurements scored 2% lower on the Mini-Mental State Examination (MMSE), a standard 30-point tool used by clinicians to screen for memory and attention deficits.
Expert Perspectives: An Early Warning Sign?
The implications of these findings are significant for how we screen for neurodegenerative risks in a post-pandemic world.
“Our work suggests that long-term immune reactions post-COVID may cause swelling that damages this critical brain barrier,” stated senior author Yulin Ge, MD, Professor of Radiology at NYU Grossman School of Medicine. Dr. Ge noted that this physical and molecular evidence suggests a larger ChP may serve as an “early warning sign” for future Alzheimer’s-like cognitive decline.
However, the medical community urges a measured interpretation of the data. Thomas Wisniewski, MD, Director of NYU Langone’s Center for Cognitive Neurology and co-senior author of the study, emphasized the need for longitudinal tracking.
“Our next step is to follow these patients to see if these brain changes actually predict long-term cognitive issues,” Wisniewski said. “A larger study will clarify if these alterations are the cause of the symptoms or a result of them.”
The Broader Context: Why the Choroid Plexus Matters
The choroid plexus is a delicate vascular network that produces protective fluid and regulates the “blood-cerebrospinal fluid barrier.” Previous research has shown that the SARS-CoV-2 virus can bind to ACE2 receptors within this structure, potentially allowing inflammatory proteins, like cytokines, to “leak” into the brain.
Long COVID is estimated to affect between 10% and 30% of survivors. For those experiencing “brain fog,” the fear has always been whether the damage is permanent. While prior studies have linked severe COVID-19 cases to a 19-fold increase in the odds of mild cognitive decline, this new research provides a specific anatomical target for where that decline may begin.
Public Health and Clinical Implications
If the choroid plexus enlargement is confirmed as a reliable biomarker, it could revolutionize how Long COVID is treated.
For Healthcare Professionals
Doctors may soon integrate brain MRIs or specific blood tests—looking for pTau217 and GFAP—into standard Long COVID protocols. Identifying patients with “clogged” plumbing early could allow for targeted interventions, such as specialized anti-inflammatory treatments, before irreversible damage occurs.
For the Public
For the average reader, the study underscores the importance of monitoring cognitive health following a COVID-19 infection. Experts recommend:
-
Vascular Health Management: Maintaining heart health through a Mediterranean diet and blood pressure control, as vascular health is inextricably linked to brain waste clearance.
-
Physical Activity: Engaging in at least 150 minutes of weekly aerobic exercise to promote healthy blood flow.
-
Vaccination: Data shows that vaccination can reduce the risk of developing Long COVID by 15% to 50%, providing a primary line of defense against these structural brain changes.
Limitations and Counterpoints
While the study is a significant step forward, it is not without caveats. As a cross-sectional study, it captures a “snapshot” in time. This means researchers cannot yet prove that COVID caused the enlargement, or that the enlargement will definitely lead to Alzheimer’s.
Furthermore, with a sample size of 179, the results may not apply to everyone. Some smaller studies have even reported inconsistent findings, with some cohorts showing smaller choroid plexus volumes, possibly due to differences in infection severity or the timing of the MRI.
“We see shared pathways of inflammation, but we must remember that dementia risk is multifactorial,” says independent experts not involved in the NYU study. “A biomarker is an association, not a destiny.”
Moving Forward
For those currently suffering from Long COVID, the news of “Alzheimer’s-like” changes may be daunting. However, the identification of a specific mechanism—the choroid plexus—gives scientists a concrete target for new therapies.
The goal now shifts from merely documenting “brain fog” to developing “plumbing” repairs for the brain.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
https://health.economictimes.indiatimes.com/news/industry/study-suggests-long-covid-alzheimers-may-share-disease-mechanisms/128330724#:~:text=Studies%20have%20shown%20that%20problems,choroid%20plexus%2C%20the%20researchers%20said.