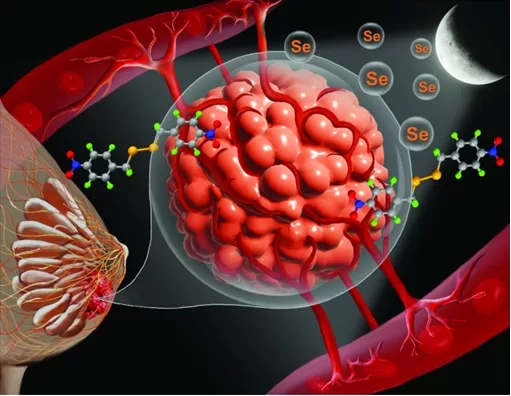
A new study in Nature reports that disabling a single “bodyguard” protein in lung cancer cells can trigger a form of cell suicide called ferroptosis, shrinking tumors in mice by up to 80% and prolonging survival. The work, led by researchers at NYU Langone Health, focuses on ferroptosis suppressor protein 1 (FSP1), and suggests this protein could become a promising new drug target for hard‑to‑treat lung adenocarcinoma, the most common type of lung cancer in people who have never smoked.
What the study found
The research team used genetically engineered mouse models of lung adenocarcinoma to “switch off” FSP1 specifically in tumor cells, which led to a marked buildup of toxic lipid by‑products and a strong slowdown in tumor growth. In these mice, tumors shrank by as much as 80% compared with controls, reflecting widespread ferroptosis—an iron‑dependent form of cell death driven by damage to fatty components of cell membranes.
To test a drug‑like approach, the scientists then used icFSP1, an experimental small‑molecule inhibitor designed to block FSP1’s activity. In multiple mouse models, treatment with icFSP1 reduced tumor burden and extended survival to nearly the same degree seen when the FSP1 gene was completely deleted, strengthening the case that FSP1 is a key survival factor for these cancer cells.
How ferroptosis works
Ferroptosis is distinct from more widely known forms of programmed cell death such as apoptosis; it is triggered when iron and “reactive oxygen species” (ROS) drive uncontrolled oxidation of lipids in cell membranes. Under normal conditions, proteins such as glutathione peroxidase 4 (GPX4) and FSP1 act as cellular “firefighters,” using antioxidant systems to neutralize lipid peroxides and keep ferroptosis in check.
The new study indicates that, in lung adenocarcinoma specifically, FSP1 appears to be especially important for suppressing ferroptosis in vivo, more so than GPX4. When FSP1 was lost or inhibited, tumors accumulated lipid peroxides, and blocking ferroptosis through genetic, dietary, or pharmacologic means restored tumor growth—clear evidence that the anti‑tumor effect depended on ferroptosis.
Why FSP1 is a particularly attractive target
Across analyses of human lung adenocarcinoma samples, higher levels of FSP1 were linked with more aggressive disease and poorer survival, whereas GPX4 levels did not show the same prognostic pattern. This suggests FSP1 is not just a passive stress‑response protein but may actively help tumors resist both natural cell‑death signals and some cancer therapies.
Crucially, the study and recent reviews indicate that FSP1 plays a relatively smaller role in normal, healthy cells compared with its role in cancer, at least in the models tested. If this holds true in humans, drugs that target FSP1 might selectively weaken tumor cells’ defences with fewer side effects than strategies that hit more universally essential antioxidant systems such as GPX4.
Expert perspective and caution
Oncologists not involved in the research say the findings are exciting but still at an early, preclinical stage. Reviews of ferroptosis‑based cancer therapies note that FSP1 has emerged as a central “hub” controlling resistance to ferroptosis across many tumor types, and that pharmacological inhibitors can, in preclinical systems, both shrink tumors and potentially enhance responses to chemotherapy or immunotherapy. However, they also emphasize that the biology of ferroptosis in humans is complex, involving iron metabolism, lipid handling, and the immune microenvironment, which may behave differently in patients than in mice.
Experts also highlight that ferroptosis is a double‑edged sword: while triggering it in cancer cells can be beneficial, inappropriate ferroptosis in healthy tissues has been linked to conditions such as neurodegeneration and organ injury in other contexts. Any future FSP1‑targeting drugs will need careful dose‑finding and safety monitoring to avoid harming normal organs that rely on finely tuned oxidative balance.
Implications for patients and public health
Lung cancer remains the leading cause of cancer‑related death worldwide, and lung adenocarcinoma accounts for roughly 40% of cases, including many diagnosed in people who never smoked. Current treatments—surgery, radiation, chemotherapy, targeted drugs, and immunotherapy—have improved outcomes for some patients, but resistance and relapse are common, making new therapeutic strategies an urgent public‑health priority.
If FSP1 inhibitors eventually prove safe and effective in humans, they could add a new class of treatments aimed not at directly damaging DNA or blocking growth signals, but at dismantling tumors’ defences against a natural cell‑death program. In principle, such agents might be combined with existing therapies to resensitize resistant tumors or reduce the doses needed of more toxic drugs, though this remains speculative until clinical trials are done.
What this means (and does not mean) for readers today
For patients and families, the main takeaway is that this research identifies a promising vulnerability in lung adenocarcinoma cells, but it has so far been demonstrated only in laboratory and animal models. IcFSP1 and related compounds are not approved cancer treatments, and there is currently no clinically available test or drug that allows patients to “turn off” FSP1 in tumors outside of research settings.
People living with lung cancer should not change their current therapies or rely on supplements or unproven products claiming to “induce ferroptosis” or “block FSP1”; such approaches are unsupported by evidence and may interfere with standard care. The most practical steps remain well‑established: prompt evaluation of symptoms, adherence to recommended treatments, participation in clinical trials when appropriate, and lifestyle measures such as smoking cessation and managing other health risks.
Study limitations and unanswered questions
Although the results are robust across several preclinical models, mouse studies do not always predict how human cancers will respond, especially over longer time frames and in the setting of other illnesses. The optimal dose, schedule, and combination partners for FSP1 inhibitors like icFSP1, as well as their potential off‑target effects, will need to be clarified in carefully designed early‑phase clinical trials.
The study also focuses on lung adenocarcinoma driven by particular genetic changes, and it is not yet clear whether all subtypes of lung cancer—or other solid tumors such as pancreatic or liver cancers—will depend on FSP1 to the same extent. Ongoing research is exploring whether modulating ferroptosis, including via FSP1, can be safely harnessed across different cancers and how best to identify patients who are most likely to benefit.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
https://health.economictimes.indiatimes.com/news/industry/blocking-a-single-protein-forces-cancer-cells-to-self-destruct-study/125474568?utm_source=top_story&utm_medium=homepage