Published: March 9, 2026
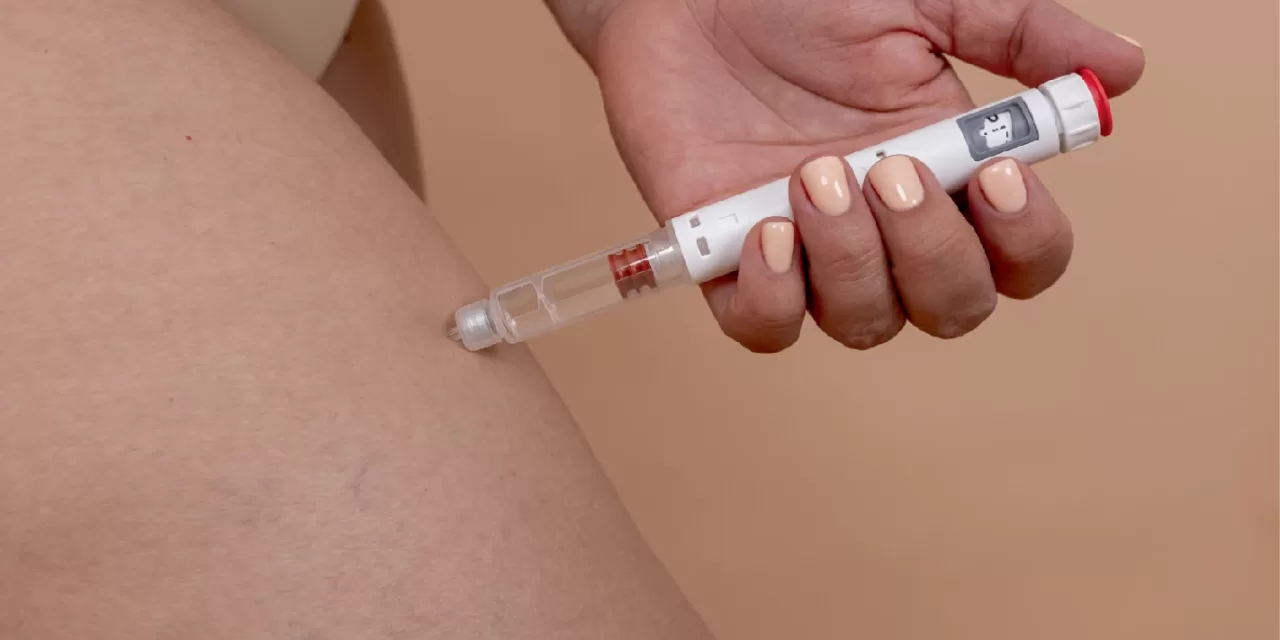
ST. LOUIS — The medications that revolutionized the treatment of obesity and type 2 diabetes are now showing “remarkable” potential to tackle another of modern medicine’s greatest challenges: substance use disorders. A massive new study of over 600,000 U.S. veterans, published in early March 2026 in The BMJ, reveals that patients taking GLP-1 receptor agonists like semaglutide (Ozempic, Wegovy) and tirzepatide (Mounjaro, Zepbound) experienced significantly lower rates of new addiction and better outcomes for existing substance-related issues.
The findings suggest these drugs do more than just slow digestion or manage insulin; they appear to “quiet” the brain’s fundamental reward pathways, reducing the biological drive for alcohol, opioids, nicotine, cannabis, and even cocaine. For a public health landscape currently ravaged by the opioid crisis and chronic alcohol misuse, the implications are profound.
A Shield Against Addiction: Key Findings
The cohort study, led by Dr. Ziyad Al-Aly of the Washington University School of Medicine, tracked a massive population of veterans with type 2 diabetes over three years. To ensure the results weren’t just a byproduct of better health management, researchers compared GLP-1 users to those taking SGLT2 inhibitors—another class of diabetes drugs that manage blood sugar but do not interact with the brain’s reward centers.
For participants who had no prior history of addiction, the GLP-1 medications acted as a significant preventive measure. The risk of developing a new substance use disorder (SUD) dropped across the board:
-
Opioid Use Disorder: 25% lower risk
-
Nicotine Dependence: 26% lower risk
-
Alcohol Use Disorder: 18% lower risk
-
Cannabis and Cocaine Disorders: Approximately 20% lower risk
Even more striking were the results for the 81,617 participants who already struggled with addiction. For these individuals, GLP-1 treatment was associated with a 39% reduction in drug overdoses and a staggering 50% fewer substance-related deaths.
Quieting the “Drug Noise”
To understand why a diabetes drug affects heroin or alcohol cravings, one must look at the brain’s “reward circuit”—the mesolimbic dopamine system. This area of the brain is responsible for the “surge” of pleasure we feel when we eat a calorie-dense meal or use an addictive substance.
GLP-1 receptors are not just in the gut; they are also located in these reward-processing centers. By mimicking a natural hormone, these drugs signal to the brain that “enough is enough.”
“People taking these drugs for obesity often describe a quieting of ‘food noise’—those intrusive, constant thoughts about eating,” explained Dr. Al-Aly. “Our study suggests something broader: GLP-1 drugs may also quiet ‘drug noise,’ the persistent cravings that drive substance use.”
Unlike traditional addiction treatments, which are often substance-specific (such as nicotine patches for smoking or naltrexone for alcohol), GLP-1s appear to target a shared biological pathway. This “universal” approach could provide a breakthrough for treating addictions to stimulants like methamphetamine or cocaine, for which there are currently no FDA-approved medications.
Expert Perspectives and Growing Evidence
The medical community is reacting with “cautious optimism.” While this is the largest study of its kind, it builds on a foundation of smaller, controlled trials.
In 2025, a study published in JAMA Psychiatry found that low-dose semaglutide significantly reduced heavy drinking days and cigarette use in adults with alcohol use disorder (AUD). Furthermore, a Swedish registry study of 227,000 patients found that those on GLP-1s were half as likely to be hospitalized for alcohol-related issues compared to those on standard treatments.
Dr. Anna Lembke, an addiction specialist at Stanford University and author of Dopamine Nation, has noted that many of her patients report a spontaneous loss of interest in addictive behaviors after starting these medications for weight loss. However, she stresses the need for more clinical trials. “The anecdotal evidence is powerful, but we need randomized, double-blind trials to move from ‘observation’ to ‘standard of care,'” Lembke says.
Public Health and Practical Implications
The potential impact on public health is staggering. In the U.S. alone, over 40 million people struggle with alcohol use disorder, and 6 million live with opioid use disorder. Current treatments have success rates often hovering between 10% and 20% long-term.
For the average reader, this research does not mean one should seek an Ozempic prescription to quit smoking—not yet. These drugs are currently only FDA-approved for type 2 diabetes and chronic weight management.
What Patients Should Know:
-
Off-label Use: Doctors may occasionally prescribe these off-label for patients with comorbid conditions (e.g., a patient with both obesity and alcohol use disorder), but insurance coverage for addiction alone is currently non-existent.
-
Side Effects: GLP-1s are not without risks. Between 20% and 40% of users experience nausea, vomiting, or gastrointestinal distress. Rare but serious risks include pancreatitis.
-
Sustainability: Much like weight loss, the “anti-addiction” effects may wane once the medication is stopped, suggesting that long-term treatment might be necessary for some.
Limitations: The Road Ahead
Despite the “remarkable” data, Dr. Al-Aly and other experts urge a measured approach. This study was observational, meaning it identifies a link, not a definitive cause-and-effect. Because the study focused on veterans—a group that is predominantly male and older—the results might not perfectly translate to the general population or younger women.
There is also the question of “motivational blunting.” Some researchers worry that by dampening the brain’s reward system, these drugs might also reduce pleasure from healthy activities, like exercise or socializing.
Looking Forward
The next two years will be critical. The National Institute on Drug Abuse (NIDA) is currently funding trials to see how semaglutide and tirzepatide affect stimulant and opioid use disorders. Another trial, NCT07292519, is investigating tirzepatide combined with behavioral therapy for patients with both obesity and alcohol use disorder.
If these clinical trials confirm what the veteran data suggests, we may be on the cusp of a new era in addiction medicine—one where a weekly injection helps “turn down the volume” on the cravings that have historically proven so difficult to silence.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
-
Al-Aly Z, et al. (2026). Glucagon-like peptide-1 receptor agonists and risk of substance use disorders among US veterans with type 2 diabetes: cohort study. BMJ. doi:10.1136/bmj-2025-086886