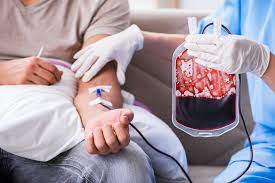
In a disturbing revelation that has sent ripples through the international medical community, reports of pediatric thalassemia patients contracting HIV following blood transfusions have surfaced, highlighting a critical breakdown in blood safety protocols. Thalassemia, a genetic blood disorder requiring lifelong, frequent transfusions, is supposed to be managed through a system of rigorous screening and high-tech filtration. However, recent cases in regional healthcare hubs have exposed “systemic lapses” within the very infrastructure designed to protect the most vulnerable.
The situation has prompted urgent calls from hematologists, patient advocacy groups, and global health experts to overhaul blood bank oversight. At the heart of the crisis is a fundamental question: In an era of advanced diagnostic testing, how are preventable infections still reaching pediatric wards?
The Thalassemia Lifeline: A Double-Edged Sword
Thalassemia is a condition where the body does not produce enough hemoglobin, the protein in red blood cells that carries oxygen. For those with Thalassemia Major, the most severe form, survival depends on blood transfusions every two to four weeks.
For children like those affected in recent reports, a blood bank is not just a medical facility; it is a lifeline. However, when screening processes fail, that lifeline becomes a vector for life-altering pathogens. HIV, Hepatitis B, and Hepatitis C remain the primary risks in what are known as Transfusion-Transmitted Infections (TTIs).
“The tragedy here isn’t just the infection; it’s the betrayal of trust in a system that these families rely on for survival,” says Dr. Elena Rossi, a senior hematologist and consultant for the Global Blood Safety Initiative (not involved in the specific cases). “A child with thalassemia is already fighting a monumental battle. Adding a chronic, stigmatized infection like HIV due to administrative or technical negligence is a public health failure of the highest order.”
Identifying the Systemic Lapses
The investigation into these recent cases points to a multi-layered failure in the blood supply chain. Experts identify three primary areas where the system collapsed:
1. The “Window Period” and Testing Limitations
While many blood banks utilize ELISA (Enzyme-Linked Immunosorbent Assay) testing, this method has a significant “window period”—the time between when a donor is infected and when the test can detect antibodies. If a donor gives blood during this window, the result may return as a “false negative.”
More advanced centers use Nucleic Acid Testing (NAT), which looks for the virus’s genetic material and significantly shrinks this window. However, NAT is expensive and not universally mandated in all regions, leading to a “safety gap” between premium urban hospitals and underfunded regional facilities.
2. Lack of Stringent Donor Screening
Technology is only as good as the human element. Systemic lapses often begin with inadequate donor questionnaires. If a high-risk donor is not properly screened out during the interview phase, the burden of safety falls entirely on the laboratory tests, which are never 100% foolproof.
3. Fragmented Oversight
In many developing healthcare sectors, blood banks operate in a fragmented environment with varying levels of accreditation. Without a centralized, digitalized tracking system for every unit of blood—from “vein to vein”—it is difficult to trace infections back to their source and prevent further units from the same donor from being used.
The Human Cost: Statistical Context
According to the World Health Organization (WHO), while 99.8% of blood donations in high-income countries are screened following basic quality procedures, that number drops significantly in lower-income regions.
In India, where some of the most recent concerns have originated, it is estimated that over 100,000 children are living with Thalassemia Major. Data from the National AIDS Control Organization (NACO) has historically shown that while TTI rates are declining, thousands of people still report contracting HIV through blood transfusions annually—a statistic that many experts believe is underreported due to the difficulty of proving the source of infection months after the fact.
Expert Perspectives: A Call for Reform
The medical community is pushing for a shift from “reactive” to “proactive” safety.
“We cannot rely on ELISA alone in 2024 for a population that receives 20 transfusions a year,” argues Dr. Arvinder Singh, a specialist in transfusion medicine. “For a thalassemia patient, the cumulative risk of a ‘one-in-a-million’ error becomes significantly higher over a lifetime of treatments. Mandatory NAT testing and leucodepletion (the removal of white blood cells) must be the gold standard, not an optional luxury.”
Conversely, some public health administrators point to the logistical challenges. Implementing NAT testing nationwide requires massive investment in infrastructure and training. There is also the concern that overly stringent rules might lead to blood shortages in regions where the donor pool is already limited.
However, advocates argue that the cost of treating a lifelong HIV infection—both in terms of medication and human suffering—far outweighs the cost of a NAT test.
What This Means for Families and Patients
For parents of children with thalassemia, these reports are terrifying. However, medical professionals urge families not to skip necessary transfusions, as the risks of severe anemia and organ failure are immediate and certain. Instead, they recommend:
-
Inquiry: Ask the treating facility if they use NAT-screened blood.
-
Leucodepletion: Ensure the blood is leucoreduced, which further lowers the risk of infections and transfusion reactions.
-
Vaccination: Ensure the patient is fully vaccinated against Hepatitis B.
-
Advocacy: Join patient support groups that lobby for blood safety legislation and centralized blood bank registries.
The Path Forward
The “systemic lapses” identified in recent reports are a wake-up call for global health authorities. To move toward “Zero-Risk” blood safety, experts suggest a three-pillar approach:
-
Universal NAT implementation for all multi-transfused patients.
-
Centralized Blood Regulatory Authorities with the power to shut down sub-standard banks.
-
Voluntary, Non-Remunerated Donation: Studies consistently show that voluntary donors have the lowest rates of TTIs compared to replacement or paid donors.
As the healthcare world watches these cases unfold, the focus remains on ensuring that the medicine intended to save a child’s life does not carry a hidden, devastating price.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References and Sources
-
Investigation Report: Ten News India – “HIV cases among thalassaemic kids: Experts warn against systemic lapses in blood banks.”