March 8, 2026
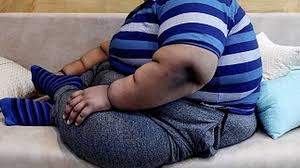
In a landmark shift in how we understand the pediatric obesity epidemic, new research suggests that the secret to a child’s healthy weight may not just be found in their lunchbox, but in their parents’ peace of mind. A groundbreaking randomized controlled trial led by the Yale School of Medicine reveals that parental stress is a primary, modifiable driver of early childhood obesity. More importantly, the study demonstrates that teaching parents mindfulness techniques can significantly stall unhealthy weight gain in high-risk children.
The study, published March 6, 2026, in the journal Pediatrics, followed 42 parent-child dyads with children aged 2 to 5. These families were identified as being at high risk for obesity, primarily hailing from low-income backgrounds where parents themselves struggled with obesity. The findings offer a powerful new tool for public health: by treating the parent’s stress, we can protect the child’s future.
The Power of a Mindful Parent
The Yale researchers divided participants into two groups. The first received standard nutrition counseling (C+N), while the second underwent a specialized mindfulness-based parent stress reduction program combined with nutrition counseling (PMH+N).
The results after just three months were stark. Children in the mindfulness group showed no significant weight increases and exhibited healthier food intake. Conversely, children in the control group—who received only nutrition advice—faced a six-fold higher risk of shifting into overweight or obesity categories during the same period.
“This trial underscores that addressing parental stress isn’t optional—it’s essential for breaking the cycle of obesity transmission in vulnerable families,” says Dr. Eliana Perrin, a pediatric obesity specialist at Duke University who was not involved in the research.
The intervention’s success was rooted in behavior. Parents in the mindfulness arm had significantly better attendance rates ($P < .015$) and reported a marked decrease in emotional eating ($P < .011$). By learning to manage their own triggers, parents were better equipped to foster a calm, structured eating environment for their children.
Why Stress Weighs So Heavily
To understand why a parent’s stress affects a child’s BMI, researchers look at the “household environment” as a biological and behavioral ecosystem. Chronic stress—stemming from financial instability, single parenthood, or lack of sleep—often forces parents into “survival mode.”
In this state, parents are statistically more likely to:
-
Model emotional eating: Children mirror their parents’ tendency to use food as a coping mechanism.
-
Rely on convenience: Stressed parents often opt for ultra-processed “fast foods” to save time and emotional energy.
-
Reduce physical activity: High cortisol levels and mental exhaustion leave little room for active play.
The biological link is equally compelling. Previous data from a 2012 study of over 2,100 families showed that for every additional major stressor a parent faces, a child’s obesity odds increase by 12%. Furthermore, perceived stress is linked to a 7% increase in the odds of frequent fast-food consumption.
“Mindfulness equips stressed parents with tools to foster better mealtime dynamics,” explains Dr. Katherine Bauer of Rutgers University. “This directly impacts child eating behaviors by reducing the chaos that often leads to overeating.”
A Growing Public Health Crisis
The implications of these findings are massive. Childhood obesity currently affects over 14 million children in the United States—a number that has tripled since the 1970s. The economic burden is equally staggering, costing the U.S. healthcare system approximately $14 billion annually.
While obesity crosses all demographic lines, it disproportionately impacts low-income and minority communities. In these populations, the stressors are often “compounded”—meaning a single family might deal with food insecurity, housing instability, and neighborhood safety concerns simultaneously. Research indicates that the stress-obesity link can be even stronger in Black and Hispanic families, where systemic inequities add layers of chronic psychological strain.
Limitations and the Road Ahead
Despite the “groundbreaking” label, experts urge a balanced interpretation of the data. The Yale study was a pilot trial with a small sample size ($n=42$) and a relatively short follow-up period of three months.
“While the results are promising, we need larger, long-term trials to see if these weight-stabilization effects hold up as children enter school age,” notes one reviewer. Critics also point out that self-reported stress measures can be subjective, and genetic predispositions to obesity still play a significant role regardless of mindfulness practices.
Practical Steps for Stressed Families
For parents feeling the weight of these findings, the message is one of empowerment, not blame. Stress is a systemic issue, but mindfulness offers a personal buffer. Health professionals recommend several low-cost strategies:
-
The Five-Minute Reset: Use free mindfulness apps for short, guided breathing exercises before high-stress periods, like the dinner rush.
-
Screen-Free Zones: Establishing “no-screen” meals helps both parents and children focus on satiety cues rather than distracting entertainment.
-
The “Toy Wait” Concept: In the study, improved “effortful control” (the ability to inhibit a dominant response) in children was a key metric. Parents can practice small “wait” games with children to build their impulse control.
-
Community Support: Seek out group-based programs. The Yale study found that the social support of the group was a major factor in why parents kept showing up.
As we move toward a more holistic view of pediatric health, the doctor’s office may soon become a place not just for weighing children, but for supporting the mental well-being of the people who raise them.
Reference Section
Primary Study:
-
Mindfulness Intervention for Parent Stress and Childhood Obesity Risk: A Randomized Trial. Pediatrics. March 6, 2026. doi:10.1542/peds.2025-072230. Lead Authors: Yale School of Medicine.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.