January 5, 2026
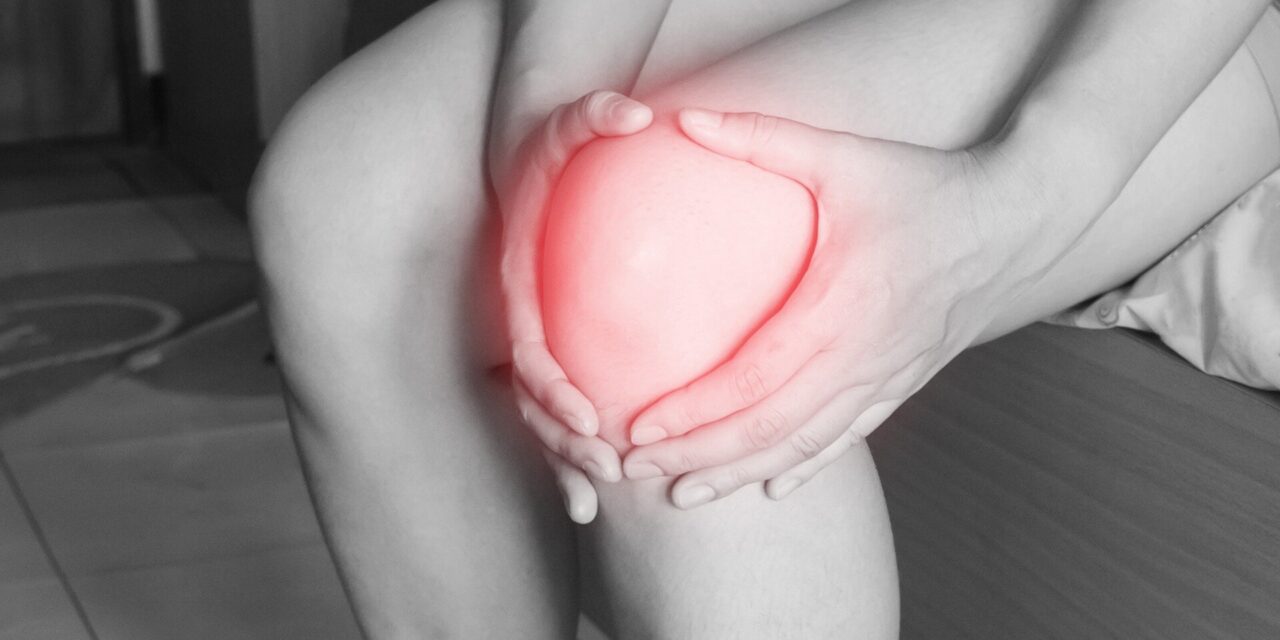
For the millions of people living with the grinding pain of “bone-on-bone” arthritis, the traditional medical roadmap has long been predictable: physical therapy, followed by steroid injections, and ultimately, a major joint replacement surgery. However, a groundbreaking study from Stanford Medicine may soon offer a third way—one that focuses on biological repair rather than mechanical replacement.
Researchers have identified a “gerozyme” (an enzyme linked to aging) that, when blocked, allows the body to naturally regrow smooth, functional knee cartilage. Published in the journal Science, the study demonstrates that a targeted injection can not only restore cartilage lost to age in mice but also prevent the onset of osteoarthritis following traumatic injuries, such as ACL tears.
Perhaps most significantly for human patients, the researchers found that human knee tissue—harvested during replacement surgeries—responded to the treatment by shifting back toward a “youthful” state and beginning to regenerate.
Targeting the “Gerozyme” Root Cause
Osteoarthritis affects approximately one in five adults in the United States, according to the Centers for Disease Control and Prevention (CDC). It carries an annual economic burden of roughly $65 billion in direct healthcare costs. Despite its prevalence, current treatments only mask symptoms.
“Until now, there has been no drug that directly treats the cause of cartilage loss,” says Nidhi Bhutani, PhD, associate professor of orthopaedic surgery at Stanford and one of the study’s senior authors.
The Stanford team focused on a protein called 15-PGDH. As we age, levels of this protein rise, acting as a “gerozyme” that degrades tissue function. Specifically, 15-PGDH breaks down prostaglandin E2, a signaling molecule that the lab of senior author Helen Blau, PhD, previously discovered is essential for tissue regeneration.
When 15-PGDH is high, prostaglandin E2 is low, and the body loses its ability to repair its “shock absorbers.” By using a small-molecule drug to block 15-PGDH, the researchers effectively took the brakes off the body’s natural regenerative processes.
A “Dramatic” Discovery in Cartilage Repair
In the study, older mice with naturally thinned cartilage received injections of the 15-PGDH inhibitor. The results were immediate and visible. The knee cartilage thickened across the joint surface, restoring a smooth gliding area.
Crucially, the treatment produced hyaline cartilage—the smooth, glossy “articular” cartilage that allows joints to move without friction. Most previous attempts at cartilage repair have resulted in “fibrocartilage,” a tougher, scarred tissue that does not function as well in the knee.
“Cartilage regeneration to such an extent in aged mice took us by surprise,” Bhutani noted. “The effect was remarkable.”
Preventing Post-Traumatic Arthritis
The study also addressed a major concern for athletes: the long-term fallout of ACL tears. While these injuries are often surgically repaired, roughly 50% of patients develop osteoarthritis within 15 years.
In the Stanford study, mice with knee injuries received twice-weekly injections for one month. These mice not only avoided developing osteoarthritis but also showed improved mobility and weight-bearing compared to untreated mice.
How It Works: Reprogramming, Not Stem Cells
One of the most surprising scientific findings was the way the tissue regrew. Usually, tissue repair relies on stem cells. However, the researchers discovered that the cartilage was regenerating through a process of “cellular reprogramming.”
The treatment caused existing cartilage cells, called chondrocytes, to change their gene expression. Specifically:
-
Inflammatory cells (which break down cartilage) decreased.
-
Regenerative cells (which build the protective matrix) nearly doubled in prevalence, jumping from 22% to 42%.
“We were looking for stem cells, but they are clearly not involved,” says Blau, who directs the Baxter Laboratory for Stem Cell Biology. “It’s a new way of regenerating adult tissue.”
| Cartilage Component | Effect of Treatment |
| 15-PGDH Protein | Reduced/Blocked |
| Prostaglandin E2 | Levels stabilized/increased |
| Hyaline Cartilage | Regeneration observed |
| Inflammation | Significantly decreased |
The Road Ahead: From Lab to Clinic
While the results in mice are promising, the application to human health is already underway. The researchers tested the inhibitor on human cartilage tissue samples removed during knee replacements. Within just one week, the human cells began to reverse their “aging” gene patterns and started forming new articular cartilage.
Furthermore, a pill-based version of this 15-PGDH inhibitor has already completed Phase 1 clinical trials for treating age-related muscle weakness. These trials showed the drug is safe and active in healthy human volunteers.
“Our hope is that a similar trial will be launched soon to test its effect in cartilage regeneration,” says Blau. “Imagine regrowing existing cartilage and avoiding joint replacement.”
Expert Perspective and Limitations
Independent experts urge cautious optimism. While the mice data is compelling, human joints are significantly larger and endure much higher mechanical loads.
“The transition from mouse models to human clinical efficacy is a significant hurdle,” says Dr. Robert Sterling (not involved in the study), an orthopaedic consultant. “We need to see if these regenerated tissues can withstand the weight-bearing demands of a human adult over several years.”
Additionally, the study utilized twice-weekly injections for a month. Determining the optimal dosing and the longevity of the repair in humans will be the primary focus of upcoming trials.
What This Means for You
For now, the treatment is not yet available for public use. However, this research marks a paradigm shift in how we view “wear and tear.” If successful in human trials, this could mean:
-
Preventative Care: Athletes could receive a short course of injections after a ligament injury to prevent future arthritis.
-
Delaying Surgery: Older adults with early-stage osteoarthritis might “regrow” their way out of needing a prosthetic joint.
-
Systemic Health: Since the protein is also linked to muscle and bone health, the treatment could potentially offer broader anti-aging benefits.
As the medical community awaits the next phase of human trials, the message is clear: the days of viewing cartilage loss as an irreversible “one-way street” may be coming to an end.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References
- https://scitechdaily.com/anti-aging-injection-regrows-knee-cartilage-and-prevents-arthritis/