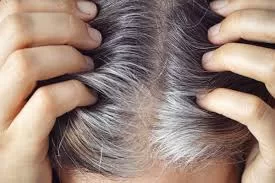
For many, alopecia areata (AA) is viewed primarily as a cosmetic challenge—a condition where the immune system mistakenly attacks hair follicles, leading to patchy or complete hair loss. However, a landmark study published late last month suggests that for many patients, particularly children and women, the scalp may only be the starting point for a broader systemic immune response.
According to research published on February 27 in the Journal of the American Academy of Dermatology, patients diagnosed with new-onset alopecia areata face a significantly higher 10-year risk of developing a range of other immune-mediated inflammatory diseases (IMIDs). The findings, which analyzed data from over 100,000 patients, highlight a critical need for long-term monitoring and specialized screening, especially in pediatric populations.
A Decade of Risk: The Study Findings
The study, led by Dr. Matthew H. Lanehart of the West Virginia University School of Medicine, utilized the massive TriNetX global health research database to track the health outcomes of 26,158 children and 77,580 adults diagnosed with AA. Researchers compared these individuals against a control group of patients with non-inflammatory hair conditions, such as telogen effluvium (temporary thinning) or trichotillosis (hair-pulling disorder).
The results revealed a startling “domino effect” of autoimmunity. Over a 10-year follow-up period, patients with AA were far more likely to be diagnosed with conditions including atopic dermatitis (eczema), autoimmune thyroiditis, psoriasis, vitiligo, and inflammatory arthritis.
The Pediatric Vulnerability
The data was particularly striking for children under the age of 18. Pediatric patients with AA showed a much higher susceptibility to secondary autoimmune conditions compared to their adult counterparts.
“This analysis demonstrates a significantly increased risk of developing several new IMIDs after an AA diagnosis,” the study authors noted. “These findings will help optimize patient screening and counseling among pediatric patients.”
Key Statistics: The 10-Year Hazard Ratio
The study used a “Hazard Ratio” (HR) to measure risk. An HR of 2.0, for example, means the group is twice as likely to develop the condition as the control group.
| Condition | Pediatric Risk (HR) | Adult Risk (HR) |
| Vitiligo | 4.61 (460% higher risk) | 3.53 |
| Autoimmune Thyroiditis | 4.21 (421% higher risk) | 1.35 |
| Psoriasis | 2.87 | 1.52 |
| Inflammatory Arthritis | 2.11 | No significant increase |
| Atopic Dermatitis | 2.02 | 1.61 |
Why Children and Females?
The study found that biological sex and age at onset play major roles in future health trajectories. Females with alopecia areata demonstrated a notably higher risk for atopic dermatitis and autoimmune thyroiditis than males. Additionally, while the risk for celiac disease was only modestly increased in children (HR 1.63), it was not found to be significantly higher in adults with AA.
Medical experts suggest that the “clustering” of these diseases occurs because they often share similar genetic pathways or “cytokine signatures”—the chemical signals the immune system uses to communicate. When the immune system is primed to attack the hair follicle, it may be more prone to attacking the thyroid gland, the skin’s pigment cells (vitiligo), or the joints.
“We are learning that the skin is often a window into the rest of the body,” says Sarah Thompson, MD, a dermatologist not involved in the study. “When we see a child with alopecia areata, we shouldn’t just be looking at their hair. We need to be looking at their thyroid labs, their skin for signs of eczema, and even asking about joint pain.”
Clinical Implications: What This Means for You
For parents of children with AA and adult women living with the condition, this study serves as a roadmap for preventive care. It suggests that a diagnosis of alopecia areata should trigger a more comprehensive health evaluation.
Practical Steps for Patients and Caregivers:
-
Regular Thyroid Screening: Given the high risk of autoimmune thyroiditis (particularly in children), periodic blood tests to check thyroid-stimulating hormone (TSH) levels may be advisable.
-
Skin Checks: Be vigilant for signs of psoriasis (red, scaly patches) or vitiligo (loss of skin pigment).
-
Monitor Joint Health: In children, persistent “growing pains” or stiffness should be evaluated for potential inflammatory arthritis.
-
Discuss the “Atopic March”: If a child has AA, discuss the risk of eczema and asthma with a pediatrician to manage symptoms early.
Limitations and Looking Forward
While the study is one of the largest of its kind, researchers noted some limitations. Because the data came from electronic health records, the severity of a patient’s alopecia areata was not always recorded. It is currently unclear if someone with a small patch of hair loss carries the same risk as someone with alopecia universalis (total body hair loss).
Furthermore, because the study relied on diagnostic codes, there is always a small possibility of misclassification. Nevertheless, the sheer size of the cohort—over 100,000 patients—provides a high level of statistical confidence in the general trends observed.
The findings underscore a shift in how the medical community views “localized” autoimmune conditions. Rather than treating hair loss in a vacuum, the modern approach is moving toward integrated, multidisciplinary care that addresses the whole person.
References
- https://www.medscape.com/viewarticle/alopecia-areata-linked-higher-risk-multiple-autoimmune-2026a10006jt
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.