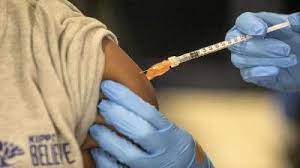
Bangladesh has launched a large-scale nationwide typhoid vaccination campaign to protect an estimated 50 million children aged between nine months and 15 years from typhoid, including increasingly drug-resistant strains. This month-long campaign started on October 12, 2025, and will continue until November 13, 2025, after which the Typhoid Conjugate Vaccine (TCV) will be integrated into Bangladesh’s routine immunization schedule. The vaccination is provided free of cost through the government’s Expanded Programme on Immunization (EPI) and is being implemented via schools, clinics, and door-to-door outreach, with a focus on vulnerable urban slums and remote rural areas. The vaccine, endorsed and pre-qualified by the World Health Organization (WHO), provides protection for up to five years with a single dose. The campaign is a critical response to the rise of drug-resistant typhoid strains in South Asia, posing a growing public health threat.
Key Developments and Context
Typhoid fever, caused by the bacteria Salmonella Typhi, spreads through contaminated food and water and leads to symptoms including prolonged fever, abdominal pain, nausea, and sometimes a rash. If untreated, it can cause serious complications including intestinal perforation and infections in other organs, which can be fatal. Bangladesh faces a high burden of typhoid, with nearly half a million cases annually and around 8,000 deaths, 68 percent of which occur among children.
A critical driver of concern is the emergence of drug-resistant typhoid strains. Over recent years, Bangladesh, along with neighboring Pakistan, has seen resistance to multiple antibiotics traditionally used to treat typhoid. Notably, Pakistan has contended with extensively drug-resistant (XDR) typhoid strains that resist nearly all antibiotics except one. Bangladesh has recorded resistance to drugs like ceftriaxone, one of the last effective treatments, and emerging resistance to azithromycin. Surveillance from 1999 to 2022 showed a decline in resistance to older first-line antibiotics but persistent high resistance to fluoroquinolones and low-level increasing resistance to third-generation antibiotics, heightening the risk of untreatable typhoid infections.
Typhoid Conjugate Vaccine (TCV) Effectiveness and Safety
The TCV used in the campaign was developed by the Serum Institute of India and is supplied through Gavi, the Vaccine Alliance. It has demonstrated strong safety and efficacy profiles in clinical studies conducted in Bangladesh and other South Asian countries. A landmark study in Mirpur, Dhaka, revealed that the TCV prevents approximately 85% of typhoid cases in vaccinated children aged 9 months to 15 years, offering immunity that lasts at least five years.
The vaccine’s safety record is robust, with no serious adverse events reported in large-scale immunization campaigns in Pakistan, Nepal, and India’s Mumbai. This builds confidence in deploying TCV widely to curtail typhoid spread and reduce reliance on antibiotics, helping to curb the surge in drug-resistant strains.
Expert Perspectives and Public Health Implications
Health Adviser Nurjahan Begum of Bangladesh inaugurated the campaign and described it as “shameful” that children still die of typhoid in Bangladesh despite success in controlling other infectious diseases like diarrhea and night blindness. She expressed optimism that the vaccine campaign would help Bangladesh overcome its decades-long battle with typhoid.
Experts emphasize that widespread TCV coverage can substantially reduce typhoid incidence and the associated morbidity and mortality, thus lightening the burden on healthcare systems. Vaccination also reduces the need for antibiotic treatments, which in turn slows the expansion of antimicrobial resistance, a growing global and regional health challenge.
For the general public, this campaign underscores the critical importance of vaccination as a preventive measure against typhoid. Besides vaccination, maintaining safe drinking water, proper sanitation, and good hygiene practices remain vital in controlling typhoid transmission.
Potential Limitations and Challenges
While TCV offers promising protection, limitations exist. The vaccine does not confer lifelong immunity, and booster doses or sustained immunization programs may be necessary. The campaign’s success hinges on achieving high coverage, especially in hard-to-reach populations such as street children and children in remote rural areas. Ensuring vaccine acceptance and overcoming logistical challenges remain critical hurdles.
Further, the emergence of drug-resistant strains, including those resistant to ceftriaxone and azithromycin, calls for continuous surveillance and research to adapt treatment protocols and develop new therapeutics. Vaccination alone cannot eliminate typhoid without addressing broader socioeconomic determinants like water quality and sanitation infrastructure.
Conclusion
Bangladesh’s ambitious typhoid vaccination drive represents a significant step towards tackling a severe and growing public health threat posed by drug-resistant typhoid. The campaign leverages the proven efficacy and safety of the WHO-prequalified Typhoid Conjugate Vaccine to protect millions of children and curb the spread of resistant bacteria. It highlights the urgency for comprehensive approaches combining vaccination, antibiotic stewardship, and improved sanitation to ultimately reduce typhoid’s burden on communities.
Medical Disclaimer: This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making any health-related decisions or changes to your treatment plan. The information presented here is based on current research and expert opinions, which may evolve as new evidence emerges.
References: