Researchers have achieved a significant milestone in diabetes treatment by successfully manufacturing insulin-producing human pancreas cells using 3D printing technology. The breakthrough, announced at the International Transplant Congress in London, could pave the way for more effective and accessible therapies for people with type 1 diabetes.
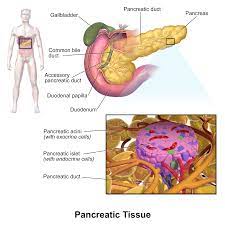
The team used a bio-ink composed of human pancreatic tissue—stripped of all cellular components—and alginate, a substance derived from seaweed, to print human pancreatic islet cells. These printed cells remained alive and functional in laboratory conditions for up to three weeks, maintaining strong insulin responses to glucose. This demonstrates their potential for future clinical applications.
One of the key advancements of this technology is the preservation of the extracellular matrix—the structural scaffold that supports cells. Traditional methods of isolating islet cells for transplantation often strip away this matrix, which can compromise cell survival and function. In contrast, the new bio-ink retains these vital components, enhancing both the survival and insulin-releasing efficiency of the printed cells.
By the 21st day in laboratory tests, the bio-printed islets showed a stronger ability to sense and react to blood sugar levels than standard islet cell preparations. They also maintained their structure without clumping or breaking down, an important factor for long-term viability.
Currently, islet cell transplants for patients with type 1 diabetes—especially those experiencing dangerous and unpredictable low blood sugar episodes—involve infusing donor islet cells into the liver. The 3D-printed islets, however, could be implanted under the skin using local anesthesia and a small incision, potentially offering a safer and more comfortable alternative for patients.
“This is one of the first studies to use real human islets instead of animal cells in bio-printing, and the results are incredibly promising,” said Quentin Perrier of Wake Forest University School of Medicine, who led the research. “It means we’re getting closer to creating an off-the-shelf treatment for diabetes that could one day eliminate the need for insulin injections”.
The research team is now conducting animal trials and exploring long-term storage options to make this therapy widely available.
Disclaimer: This technology is still in the experimental phase and has not yet been approved for clinical use in humans. Further research, including animal and human trials, is required to determine its safety and efficacy. Individuals should not interpret these findings as an immediate alternative to current diabetes treatments.